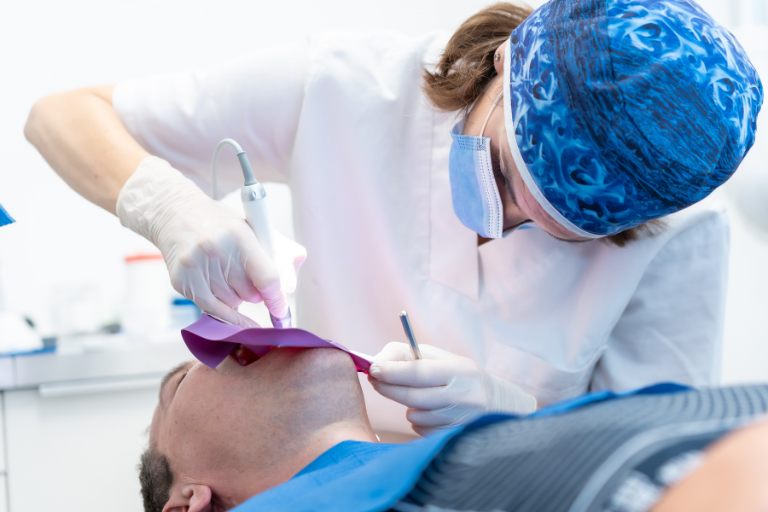
What Causes Tooth Infections That Lead to Root Canals?
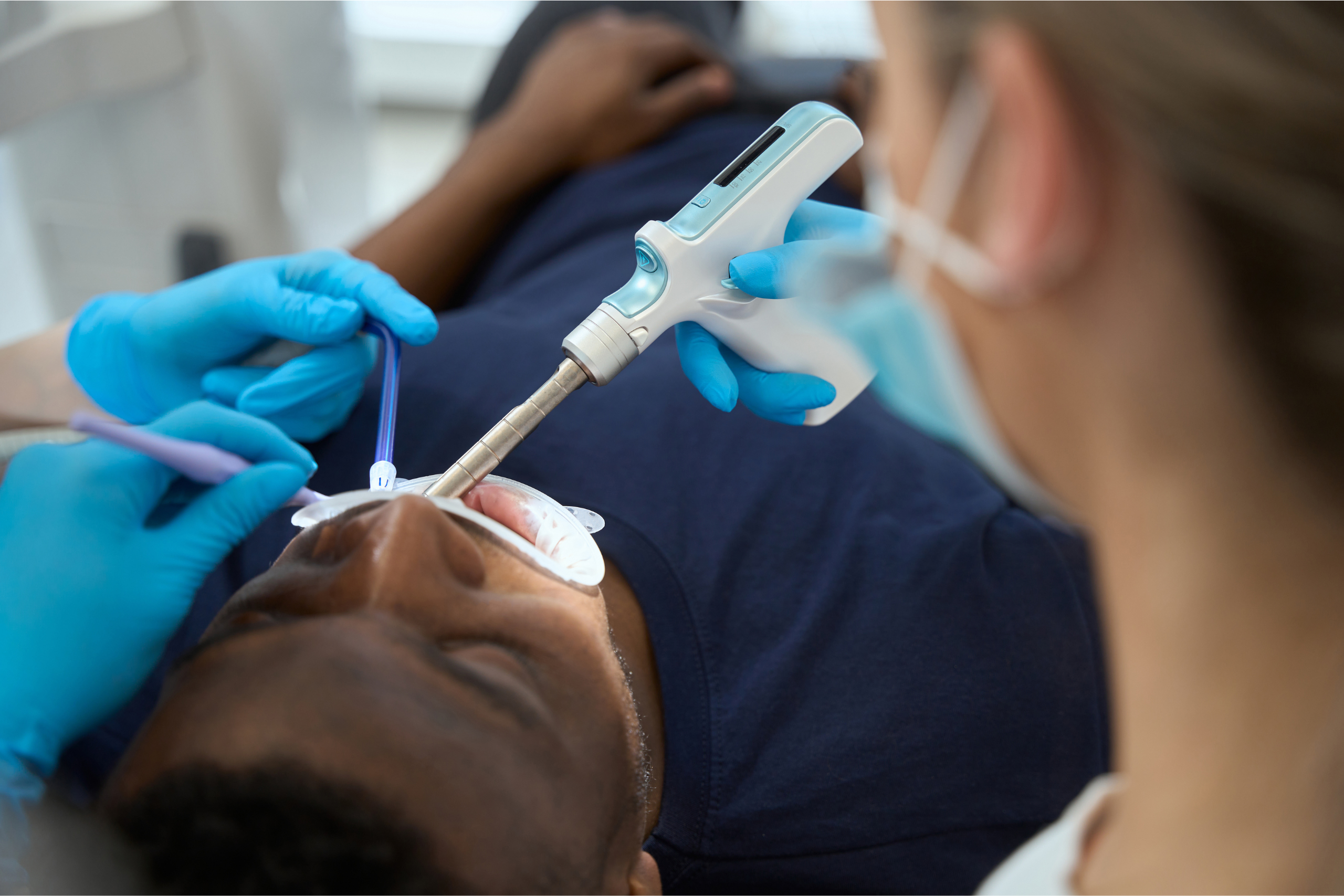
A tooth infection, also known as a dental abscess, is one of the most common reasons patients require a root canal. These infections occur when harmful bacteria invade the inner layers of a tooth, causing inflammation, pain, and damage that can only be resolved through professional treatment. Understanding what causes tooth infections can help you take preventive steps and seek care early, before significant damage occurs. For patients experiencing persistent tooth pain or sensitivity, timely evaluation is essential, and options such as root canal therapy in Scottsdale can help save the natural tooth and restore oral health.
Deep Decay From Untreated Cavities
The most frequent cause of a tooth infection is deep dental decay. When cavities go untreated, bacteria eat away at the enamel and dentin layers of the tooth, eventually reaching the pulp—the area containing nerves and blood vessels. Once bacteria invade this inner chamber, infection can spread quickly. Symptoms may include sharp pain, lingering sensitivity to hot or cold foods, or swelling in the gums. Early dental checkups and timely fillings can prevent decay from advancing into the pulp.
Cracked or Chipped Teeth
Even a small crack or chip in a tooth can create an entry point for bacteria. Some cracks are noticeable, but others may be microscopic and only visible to a dentist during an examination. Trauma from chewing hard foods, accidents, or grinding teeth can weaken tooth structure over time. When bacteria slip through these openings, they can reach the pulp and cause infection. Wearing a mouthguard at night and avoiding extremely hard foods can reduce the risk of fractures that may lead to complications.
Gum Disease (Periodontitis)
Advanced gum disease is another major contributor to tooth infections. As gum tissue pulls away from the tooth, pockets form that trap bacteria. If these pockets deepen and remain untreated, the infection can travel to the root, reaching the tooth’s interior. Periodontitis may cause bleeding gums, bad breath, gum recession, and tooth mobility. Regular cleanings and proper oral hygiene can reduce the risk of gum-related infections that ultimately require root canal treatment.
Failed or Old Dental Work
Dental fillings, crowns, and other restorations can wear down or become damaged over time. When this occurs, small gaps or leaks may develop, allowing bacteria to enter the tooth structure. A compromised restoration often goes unnoticed until symptoms appear. Regular dental checkups help ensure older dental work remains intact and continues to protect your tooth effectively.
Weakened Immune System and Poor Oral Hygiene
Individuals with weakened immune systems—such as those with chronic illnesses or high stress may be more susceptible to infections. Poor oral hygiene can also accelerate bacteria buildup, leading to plaque, tartar, and decay. Brushing twice daily, flossing, and visiting your dentist every six months significantly reduces the risk of infections that could lead to root canal treatment.
Protecting Your Smile From Tooth Infections
Tooth infections often develop silently before pain becomes noticeable, making prevention and early detection essential. If you experience persistent toothache, sensitivity, swelling, or a bad taste in your mouth, don’t ignore the symptoms; these may indicate an active infection. Seeking prompt dental care can prevent the infection from worsening or spreading. Many patients find relief through advanced treatments such as root canal therapy in Scottsdale, which can eliminate infection and preserve the natural tooth.
For compassionate, high-quality care, Pinnacle Peak Dentistry offers comprehensive solutions to diagnose and treat tooth infections before they cause lasting damage. If you’re experiencing symptoms or want to protect your oral health, we encourage you to request an appointment today.
FAQs
Tooth infections typically develop when bacteria enter the inner pulp of a tooth due to deep decay, cracks, gum disease, or failing dental restorations. Once the pulp becomes infected, a root canal is often needed to remove bacteria and save the natural tooth.
Untreated cavities allow bacteria to eat through the enamel and dentin until they reach the pulp. When infection reaches this inner layer, it can cause severe pain, swelling, and the need for root canal treatment.
Yes. Cracks and chips create openings where bacteria can enter the tooth. Even small or unseen fractures may allow infection to develop over time, eventually requiring a root canal.
Advanced gum disease can cause deep pockets around the teeth, which trap bacteria. If infection spreads to the roots or pulp, it may lead to inflammation that requires root canal therapy to resolve.
Worn or damaged dental restorations can develop small gaps that let bacteria leak into the tooth. This can lead to decay beneath the restoration and eventually cause infection in the pulp.
Common symptoms include persistent toothache, swelling, sensitivity to hot or cold temperatures, gum tenderness, bad breath, or a bad taste in the mouth. In advanced cases, patients may also notice facial swelling.
Yes. Maintaining good oral hygiene, attending regular dental checkups, treating cavities early, and protecting teeth from injury can significantly reduce the risk of infection and root canal treatment.